Overview
This article outlines best practices for conducting trials of breakthrough medical devices, highlighting the critical role of early stakeholder engagement, adaptive study designs, and patient-centric approaches in enhancing trial outcomes. By detailing how these strategies streamline execution, improve recruitment and retention rates, and ultimately facilitate quicker market access for innovative medical technologies, it underscores the significance of collaboration. Successful partnerships and regulatory insights from industry leaders further support these claims, demonstrating the effectiveness of these approaches in the Medtech landscape.
Introduction
In the realm of healthcare innovation, breakthrough medical devices possess transformative potential, paving the way for more effective treatments and improved patient outcomes. These devices, defined by their ability to address life-threatening or irreversibly debilitating conditions, stand at the forefront of a rapidly evolving medical landscape.
The FDA's Breakthrough Devices Program plays a crucial role in expediting their development and ensuring timely access for patients, reflecting a growing recognition of the need for swift innovation.
As the demand for advanced medical technologies surges, understanding the intricate processes involved in clinical trials—from regulatory compliance to patient recruitment—becomes essential.
This article delves into the multifaceted world of breakthrough medical devices, exploring their significance, the challenges faced during clinical trials, and the collaborative efforts required to bring these life-saving innovations to market.
Understanding Breakthrough Medical Devices: Definition and Importance
Breakthrough medical instruments are defined as those that provide more effective treatment or diagnosis for life-threatening or irreversibly debilitating diseases. The FDA's Breakthrough Devices Program is designed to expedite the development and review of these innovative products, ensuring that patients have timely access to therapies that can significantly improve their quality of life. This program has seen a notable increase in activity, with over 30 Step designations requested in 2022, of which 14 were granted, highlighting the growing recognition of the need for rapid innovation in medical technology.
Grasping the significance of breakthrough innovations is essential, as they frequently symbolize major progress in medical technology, tackling unfulfilled healthcare requirements and improving patient outcomes. For instance, tools that incorporate novel technologies, such as artificial intelligence or advanced biomaterials, have the potential to transform treatment paradigms. Clinical studies for these instruments, considered as trials for breakthrough medical devices, must be carefully crafted to accommodate their unique features, ensuring that the information gathered is robust and pertinent.
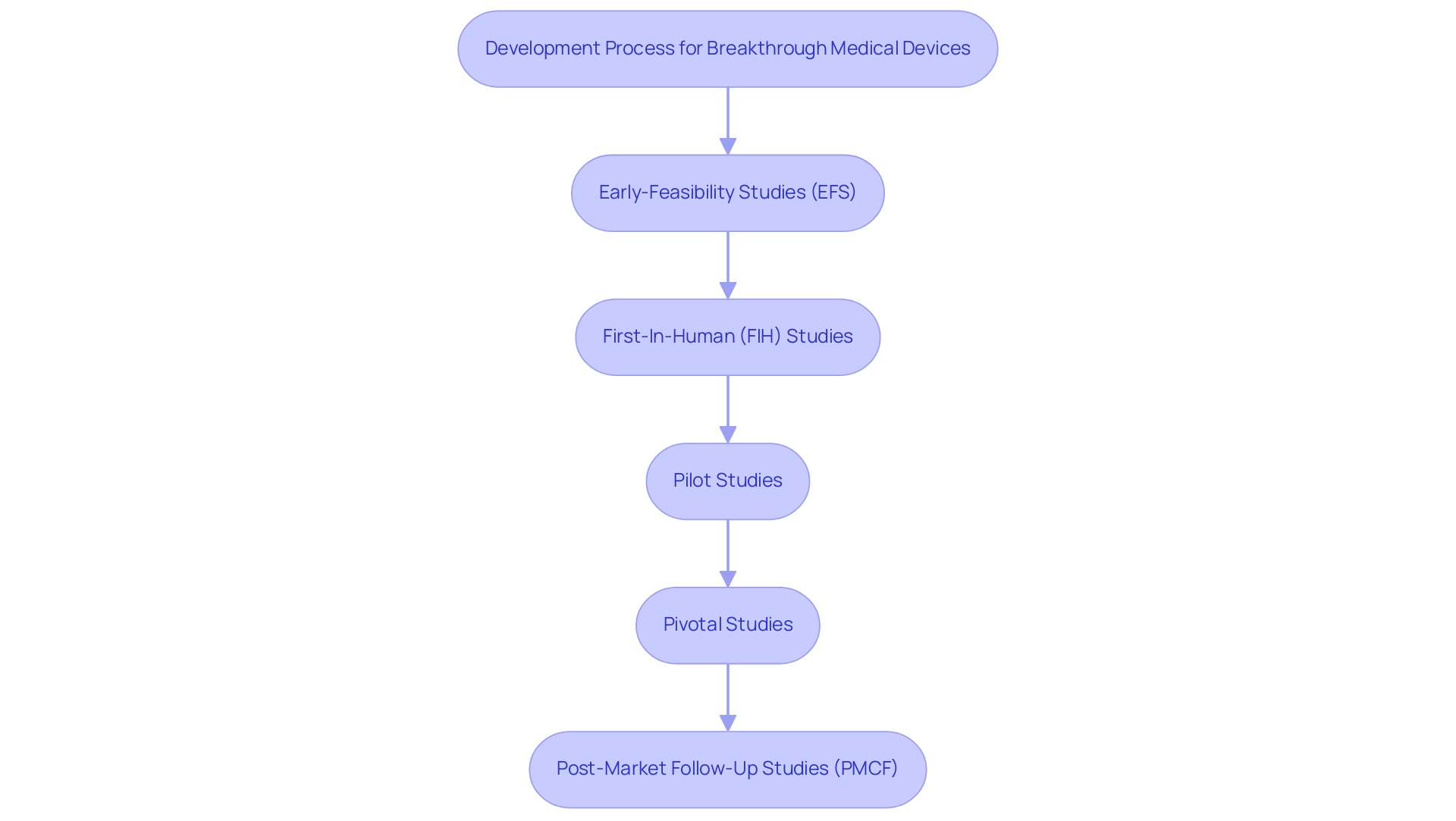
Companies like bioaccess® specialize in comprehensive trial management services, including:
- Early-Feasibility Studies (EFS)
- First-In-Human (FIH) studies
- Pilot Studies
- Pivotal Studies
- Post-Market Follow-Up Studies (PMCF)
These services are essential for navigating the complexities of regulatory approvals and ensuring successful outcomes.
Recent updates from the FDA suggest that companies should apply for Breakthrough Device Designation as soon as they can provide initial trial information demonstrating the feasibility of their device's performance in trials for breakthrough medical devices. This typically occurs after conducting trials for breakthrough medical devices that involve a limited number of clinical subjects. Prompt submission of requests after obtaining preliminary data can significantly enhance the chances of receiving the designation and expedite the overall approval process.
As Sarah Fitzgerald, Senior Consultant at Emergo by UL, noted, "CDRH is allowing some hearing aids, intended for mild to moderate hearing loss... to be sold over-the-counter (OTC) without the need for physician involvement," which reflects the evolving regulatory landscape.
The impact of groundbreaking medical instruments on patient outcomes is profound. Statistics indicate that these tools not only enhance treatment efficacy but also result in higher patient satisfaction and quality of life. Furthermore, the execution of clinical trials in regions like Latin America, supported by companies such as bioaccess®, contributes to local economies through job creation and healthcare improvements, fostering international collaboration.
However, challenges remain, such as inconsistent coverage from private insurers and the lack of approved bills for immediate CMS coverage, which can hinder access to these vital innovations. These barriers are crucial to consider, as they can significantly impact the availability of groundbreaking solutions to patients who require them the most.
In summary, breakthrough medical instruments play a pivotal role in advancing healthcare. Their development and successful integration into medical practice are essential for addressing critical health challenges and improving patient care. As the landscape of medical technology continues to evolve, the significance of these instruments in research cannot be overstated.
Navigating Regulatory Requirements for Clinical Trials
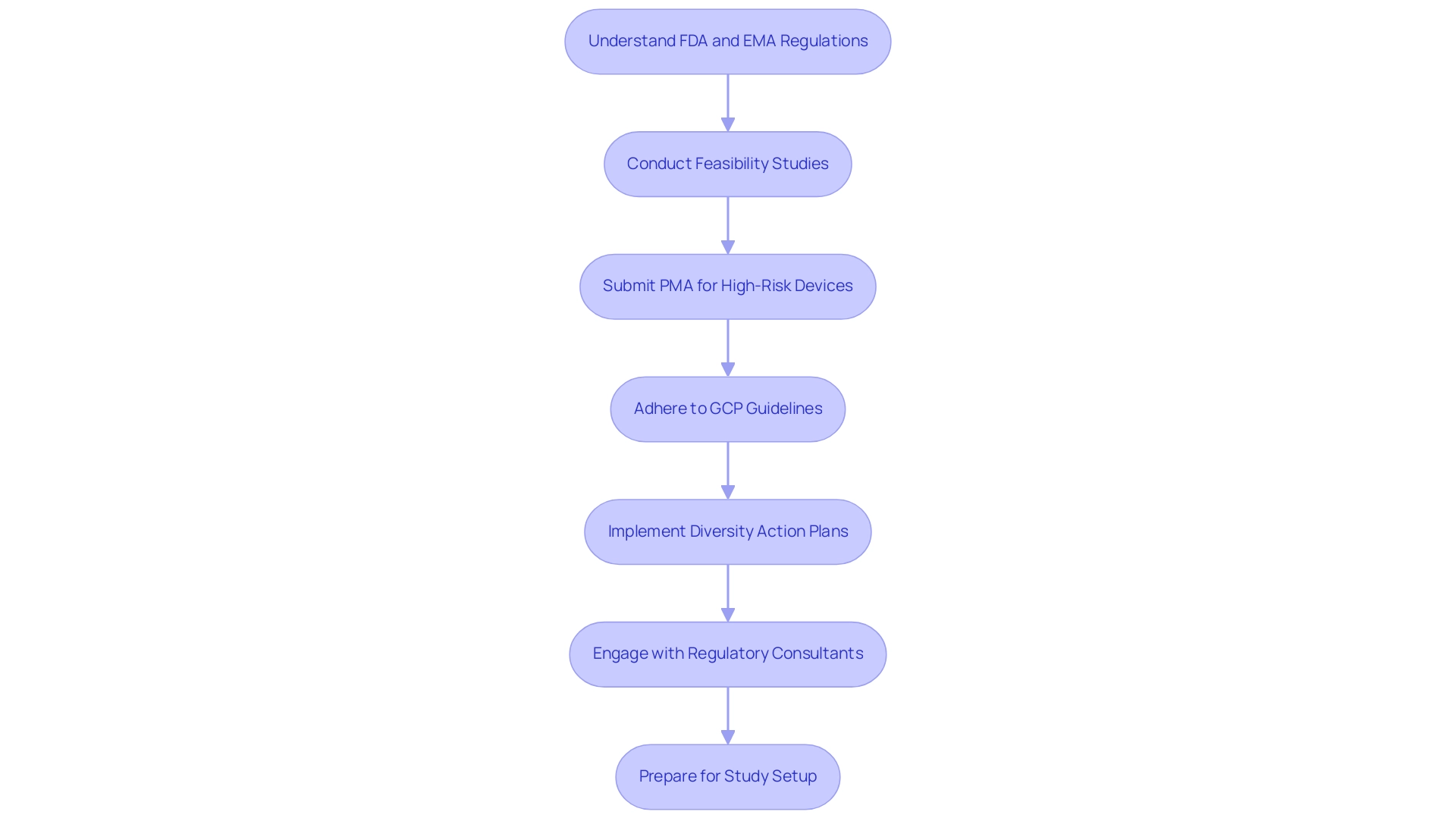
Navigating the regulatory environment for research studies requires a comprehensive understanding of the requirements set forth by regulatory bodies such as the FDA and EMA. Key regulations include the necessity for premarket approval (PMA) for high-risk devices and strict adherence to Good Clinical Practice (GCP) guidelines. With over 15 years of experience in the Medtech sector, bioaccess® emphasizes that staying informed about evolving regulations is essential, as non-compliance can result in significant delays and challenges in the research process.
In 2025, the FDA introduced updated regulations that underscore the importance of diversity in research trials, mandating sponsors to submit Diversity Action Plans (DAPs) to enhance participant enrollment from historically underrepresented populations. This initiative not only aims to improve the reliability of data but also ensures that studies reflect the demographics of the populations that will ultimately utilize these medical devices. As noted by Matthew Herper, "Scientists have concentrated on the issue of diversity in research studies both because lacking a diverse population can lead to skepticism from patients who could benefit from medicines and because some drugs do function differently in individuals of varied backgrounds."
The FDA's Breakthrough Devices Program further fosters innovation by permitting more flexible research study designs for breakthrough medical devices, which can significantly accelerate the approval process. Additionally, sponsors are required to outline strategies for achieving enrollment and retention goals, including community engagement and cultural competency training for researchers. Engaging regulatory consultants early in the study design phase is vital; their expertise can ensure that all necessary documentation and compliance measures, including review and feedback on study documents to meet country requirements and reporting on serious and non-serious adverse events, are meticulously addressed, paving the way for a smoother approval process.
At bioaccess®, our comprehensive research study management services encompass:
- Feasibility studies
- Site selection
- Compliance reviews
- Study setup
- Import permits
- Project management
- Reporting
Under the guidance of experts like Katherine Ruiz, who specializes in Regulatory Affairs for medical products and in vitro diagnostics in Colombia, we are dedicated to transforming lives in Latin America through advanced medtech. By applying these best practices and prioritizing community involvement, research teams can enhance their likelihood of success in navigating the complex regulatory landscape while also considering the emotional impacts on participants.
The Role of Collaboration in Advancing Clinical Trials
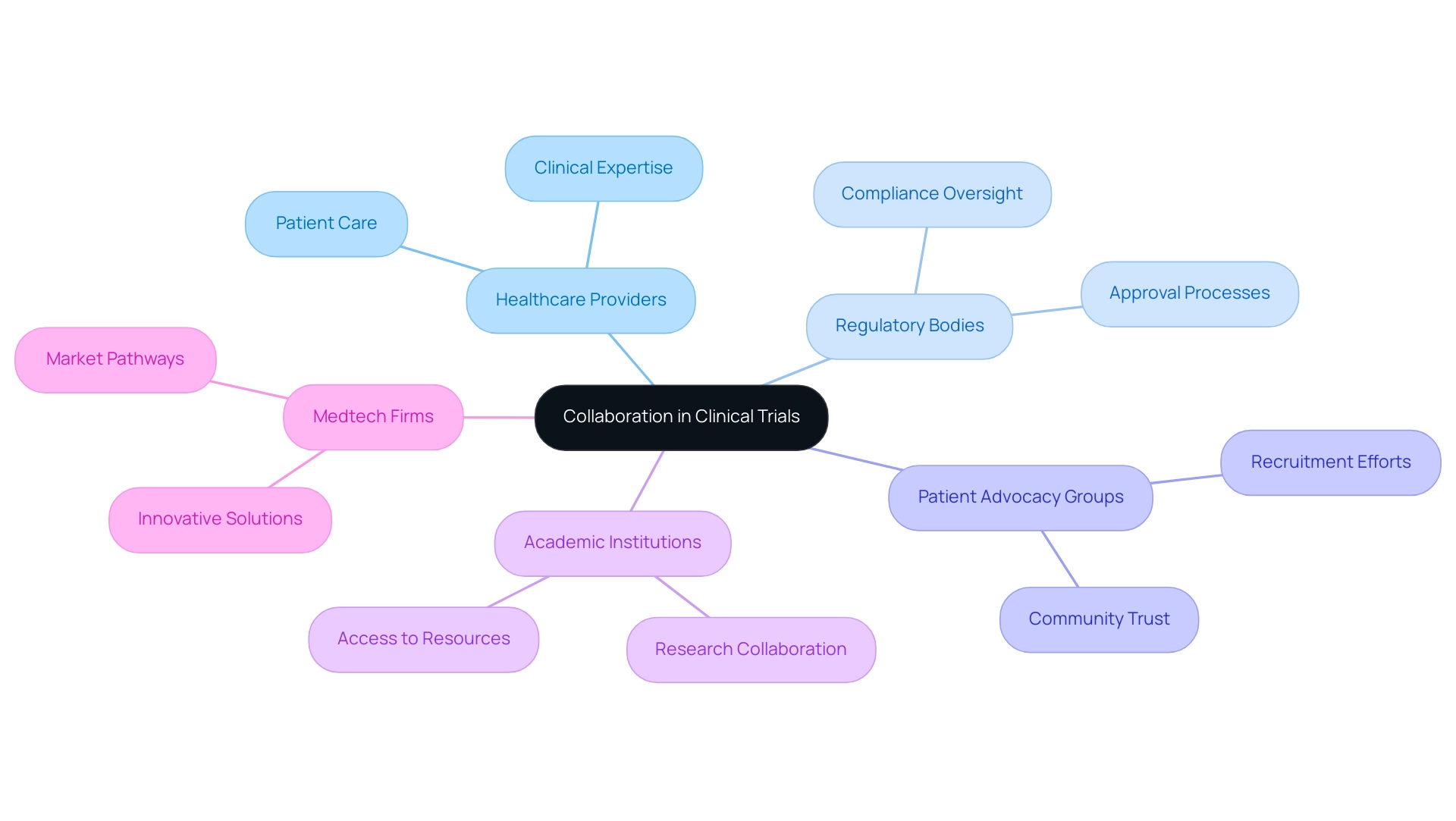
Cooperation serves as a fundamental pillar for the success of medical studies, particularly regarding breakthrough medical devices. Engaging a diverse array of stakeholders—including healthcare providers, regulatory bodies, and patient advocacy groups—can significantly enhance the research process. A notable instance is the partnership between bioaccess™ and Caribbean Health Group (CHG), which aims to establish Barranquilla as the premier location for medical studies in Latin America.
This initiative, backed by Colombia's Minister of Health, Juan Pablo Uribe, was revealed on March 29, 2019, and seeks to attract more research projects to the region, thereby fostering a robust research atmosphere. Furthermore, collaborations with academic institutions not only provide access to specialized knowledge but also leverage additional resources that can streamline study execution. Collaborations with patient organizations play a crucial role in enhancing recruitment efforts; they raise awareness and cultivate trust within communities, which is vital for participant engagement. For example, Global Care Clinical Trials' partnership with bioaccess™ has resulted in an impressive over 50% reduction in recruitment time and a remarkable 95% retention rate, underscoring the effectiveness of strategic alliances in research.
Establishing clear communication channels and aligning shared goals among all parties involved is essential for nurturing a collaborative environment. This approach not only fosters innovation but also enhances efficiency in medical studies. Research indicates that effective communication between sponsors and collaborators is vital for success, reinforcing the notion that regional coherence positively influences outcomes.
As Johnson observed, approximately 80% of research studies fail to meet their initial enrollment targets and schedules, resulting in a loss of $8 million in revenue each day for pharmaceutical development firms. This highlights the urgency and significance of cooperation in accelerating research for medical devices, particularly considering that trials for breakthrough medical devices can take an average of 10 to 15 years to develop.
Data from registered studies reveals that while 77% of studies are interventional, only 10% focus on devices, emphasizing the necessity for targeted collaboration in this domain. The global CRO market is projected to expand significantly by 2032, indicating a growing demand for research services. Successful collaborations between medtech firms and educational organizations exemplify how strategic alliances can lead to improved study outcomes and expedited pathways to market for innovative medical technologies, especially through trials for breakthrough medical devices.
Dushyanth Surakanti, Founder & CEO of Sparta Biomedical, shared his positive experience with bioaccess® during its initial human testing in Colombia, further highlighting the impact of such partnerships on advancing medical research.
Effective Patient Recruitment Strategies for Clinical Trials
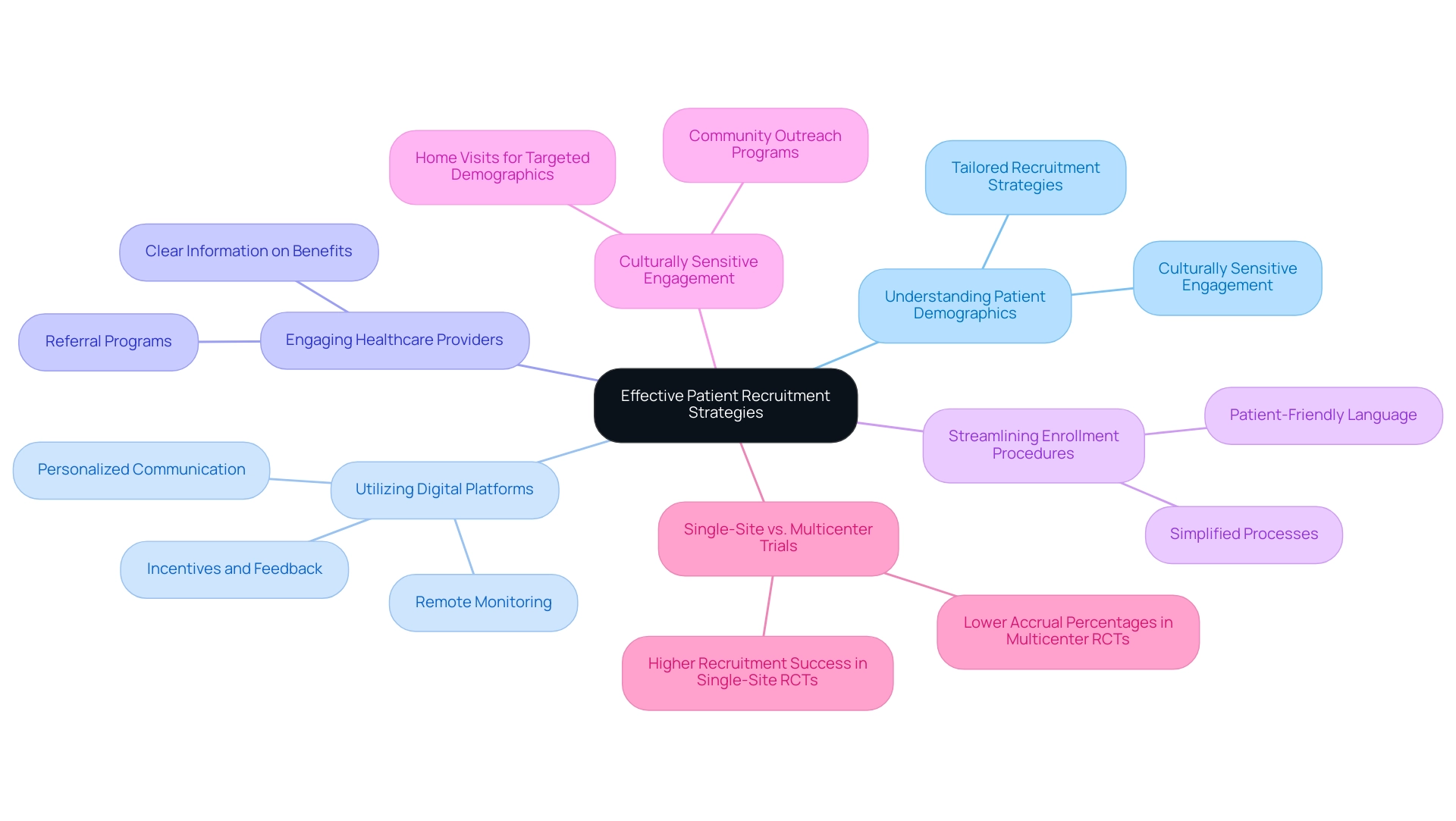
Patient recruitment remains one of the most formidable challenges in trials for breakthrough medical devices, particularly in the clinical studies sector. To optimize recruitment efforts, it is crucial to implement targeted strategies that resonate with potential participants. Understanding the demographics and motivations of the patient population is foundational; research indicates that products developed with engaged patients are more likely to succeed in the market, underscoring the importance of tailoring recruitment strategies to meet these needs.
Utilizing digital platforms for outreach has proven effective in enhancing patient enrollment. Innovative approaches, such as personalized communication and remote monitoring, have shown to significantly improve retention rates. Strategies that include offering incentives and feedback to participants can foster a more engaging experience, ultimately leading to higher enrollment success.
Engaging healthcare providers to refer eligible patients is another vital component of a successful recruitment strategy. Streamlining the enrollment procedure and offering clear, accessible information about the advantages can ease potential participants' worries. Using patient-friendly language in recruitment materials and providing flexible participation options are practical measures that can result in significant enhancements in enrollment rates.
A case study exploring the role of multicenter research in randomized controlled studies highlights that while multicenter studies can introduce complexities, single-site RCTs often attain higher recruitment success due to streamlined processes. Specifically, multicenter RCTs are associated with lower accrual percentages, indicating that individual sites may recruit more effectively in single-site studies. This insight suggests that future study designs may benefit from focusing on single-site research to enhance participant accrual.
As we look toward 2025, the landscape of patient recruitment continues to evolve. Current statistics reveal that effective recruitment strategies can yield success rates significantly higher than traditional methods. By utilizing digital platforms and comprehending the distinct motivations of various patient groups, medical studies can not only achieve their recruitment objectives but also facilitate trials for breakthrough medical devices.
Additionally, with bioaccess's extensive research management services—including feasibility studies, site selection, compliance reviews, and project management—there is a strong framework established to support these efforts. It is noteworthy that home visits have shown a greater appeal to Hispanic and non-white individuals, which highlights the need for culturally sensitive engagement strategies in recruitment efforts. This approach not only enhances recruitment but also positively impacts local economies through job creation and healthcare improvement.
Innovative Methodologies for Conducting Clinical Trials
Innovative methodologies are essential for the successful execution of trials for breakthrough medical devices. Among these, adaptive study designs stand out due to their capacity to incorporate modifications based on interim results, significantly enhancing the flexibility and efficiency of the research process. This approach has gained traction, particularly amidst recent health crises, where trials for breakthrough medical devices frequently employed adaptive platform designs and seamless layouts to optimize study outcomes during the coronavirus disease 2019.
At bioaccess®, we leverage over 20 years of expertise in managing research studies, focusing on:
- Early-Feasibility Studies
- First-In-Human Studies
- Pilot Studies
- Pivotal Studies
- Post-Market Follow-Up Studies
Our comprehensive research management services encompass:
- Feasibility studies
- Site selection
- Compliance assessments
- Study setup
- Import permits
- Project oversight
- Reporting
This ensures that each study is conducted with precision and regulatory excellence.
The integration of digital health technologies further amplifies the effectiveness of trials for breakthrough medical devices. Tools such as remote monitoring and telehealth not only enhance patient engagement but also streamline data collection processes. For instance, the utilization of wearable devices facilitates real-time tracking of patient outcomes, offering valuable insights while alleviating the burden on participants.
This shift towards innovative approaches accelerates the testing process and aligns with the evolving landscape of healthcare delivery, ensuring that research remains responsive to the needs of patients and providers alike.
Moreover, case studies have underscored the critical necessity for training in adaptive study designs among healthcare providers and researchers conducting trials for breakthrough medical devices. Findings from the case study titled "Need for Training in Adaptive Trial Designs" indicate that proper guidance and immersive training can optimize the implementation of these methodologies, ensuring that the advantages of adaptive designs are fully realized in clinical research. As noted by Professor Salaheddin M Mahmud, expert insights highlight the significance of adaptive study designs in improving outcomes.
By minimizing operational bias through rigorous planning, transparency, and comprehensive reporting, the integrity of research findings can be upheld, ultimately leading to more reliable and impactful results in the medical equipment sector. Furthermore, addressing inconsistencies in study conduct across different stages is vital for maintaining the validity of findings, emphasizing the need for meticulous management of eligibility criteria and patient recruitment.

Data Management and Analysis: Ensuring Reliable Outcomes
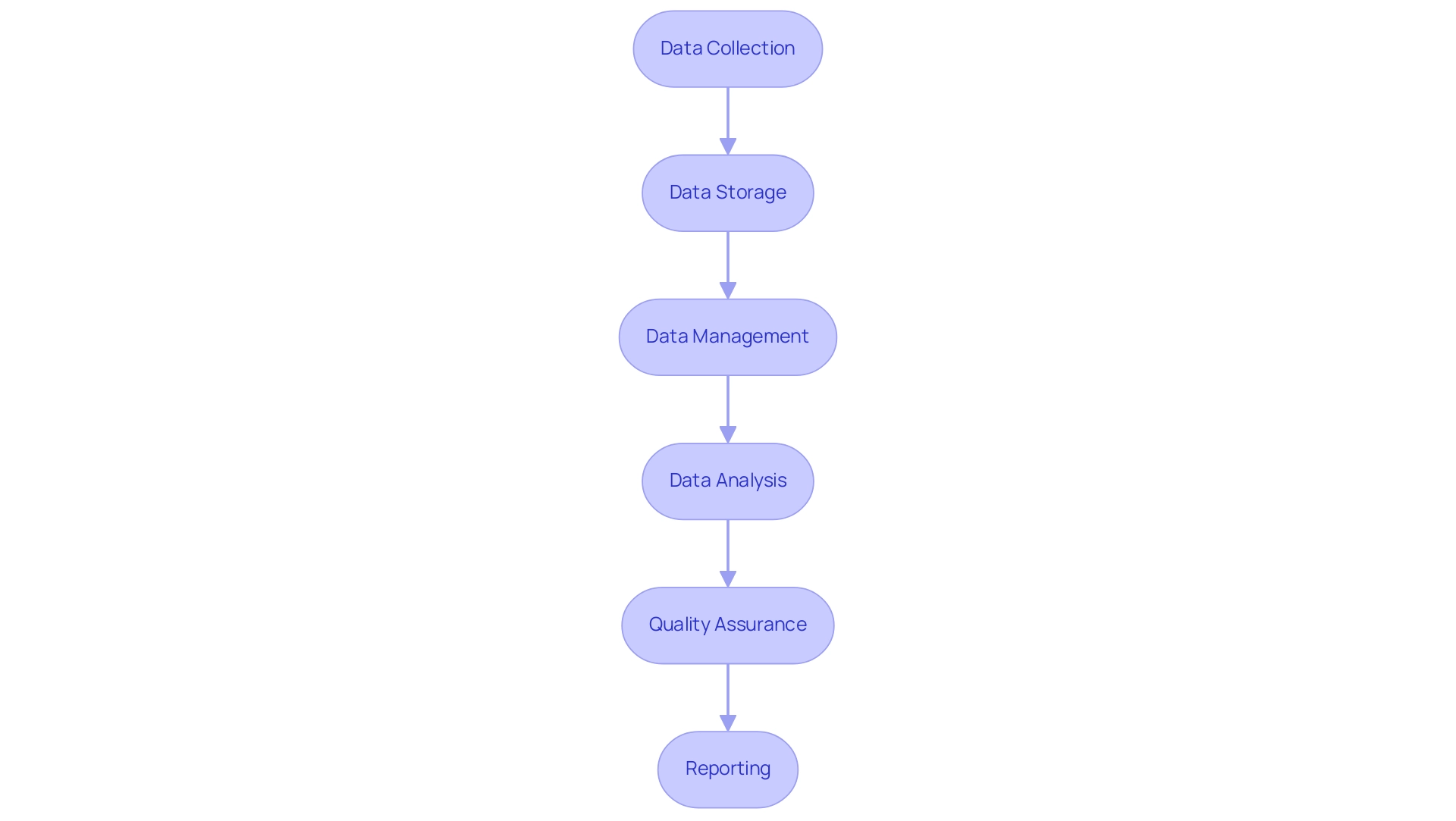
Efficient information handling and evaluation are pivotal for ensuring the reliability of medical research results, particularly concerning the expedited medical device research services provided by bioaccess® in Latin America. With over 20 years of experience in Medtech, bioaccess® employs a well-established management system for medical information, defined as specialized software applications that facilitate the collection, storage, and management of research data, significantly enhancing the processes of information gathering, validation, and reporting. Establishing clear protocols for information entry, monitoring, and quality assurance is essential to minimize errors and uphold compliance with regulatory standards.
As we approach 2025, the significance of information management in research studies is underscored by the increasing reliance on electronic information capture (EDC) systems, which enhance accuracy and enable real-time oversight of study progress. These systems are crucial not only for ensuring integrity in trials for breakthrough medical devices but also for supporting complex validation and cleaning processes, thereby improving overall trial efficiency and compliance. As Michael Young, Co-Founder, aptly states, "The significance of clinical information management cannot be overstated."
Furthermore, the integration of advanced statistical methods for analysis is vital for bolstering the robustness of findings. For instance, utilizing machine learning algorithms to analyze intricate datasets can unveil patterns that traditional analytical methods might overlook. This approach leads to more informed conclusions regarding the safety and efficacy of medical products, particularly in the context of bioaccess®'s expertise in Early-Feasibility, First-In-Human, Pilot, Pivotal, and Post-Market Follow-Up Studies, as well as trials for breakthrough medical devices.
Current trends indicate a shift towards patient-centric data management, with an increasing emphasis on real-world evidence. As the landscape of medical studies evolves, the adoption of innovative CDMS solutions, alongside advancements in technology such as artificial intelligence and machine learning, will be instrumental in enhancing study results and accelerating the journey to market for groundbreaking healthcare products. Bioaccess®'s flexibility and customized approach further solidify its position as a leader in Medtech research in Latin America, ensuring that trials for breakthrough medical devices are tailored to meet specific client needs and objectives.
Post-Market Clinical Follow-Up: Assessing Long-Term Impact
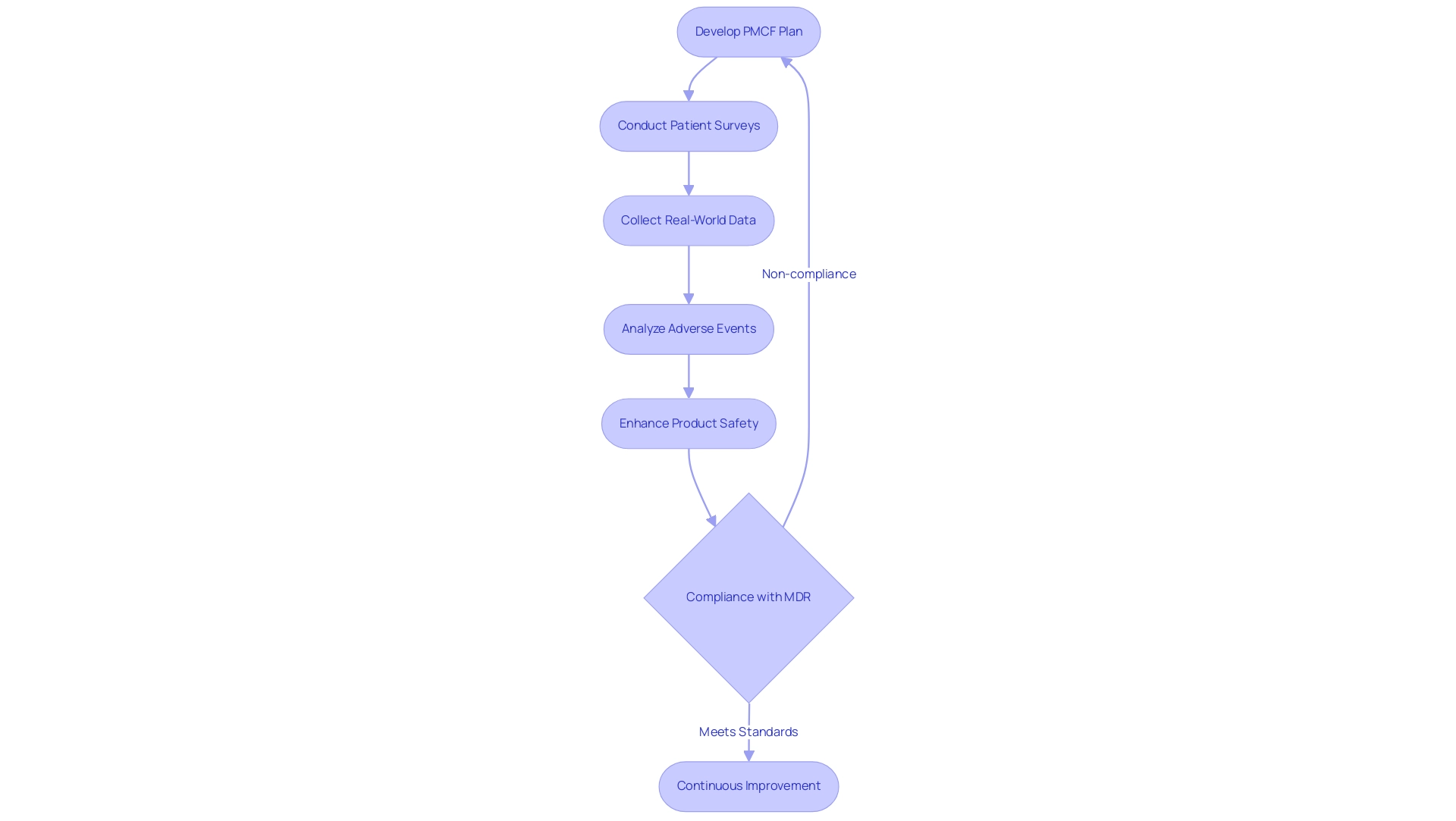
Post-market clinical follow-up (PMCF) is a vital component in the lifecycle management of medical instruments, serving as a systematic method to gather information on performance in real-world environments. This ongoing monitoring is essential for ensuring the safety and effectiveness of medical products after they have entered the market. A well-structured PMCF plan established prior to market entry not only aids in compliance with regulatory requirements, such as the Medical Device Regulation (MDR) for CE marking, but also provides invaluable insights into long-term outcomes.
Proactive data collection methods, including patient surveys and feedback mechanisms, can uncover potential issues that may not have been evident during initial trials. This approach enhances patient safety while fostering continuous improvement for future versions of the tool. Statistics indicate that effective PMCF practices can significantly reduce the incidence of adverse events, thereby improving overall safety metrics.
At bioaccess®, our expertise in PMCF is complemented by our commitment to innovation and regulatory excellence in the Medtech sector, backed by over 20 years of experience. We specialize in managing a range of studies, including Early-Feasibility Studies (EFS), First-In-Human Studies (FIH), Pilot Studies, and Pivotal Studies, ensuring a comprehensive approach to clinical research. Expert views emphasize the importance of PMCF in the medical equipment lifecycle, and industry leaders support the incorporation of real-world information (RWI) collection strategies, despite obstacles such as variability in quality and inconsistent coding.
A recent case study highlighted the difficulties in utilizing electronic health records (EHRs) for RWD collection, revealing issues like missing information and the necessity for longitudinal follow-up across multiple healthcare systems. Nevertheless, the study successfully captured performance failures and adverse events, aligning with treatment guidelines, and emphasized the need for improved data querying methods and AI assistance for better analysis. This underscores the significance of creating strong PMCF plans that can tackle these challenges efficiently.
In 2025, best practices for PMCF will continue to evolve, emphasizing the necessity of developing robust PMCF plans that enhance safety and efficacy. By prioritizing these practices, manufacturers can ensure that their products not only meet regulatory standards but also contribute positively to patient outcomes over the long term. Adhering to the MDR’s post-market monitoring requirements is crucial for manufacturers to secure and uphold the CE marking for their products.
Additionally, as noted by Dr. Nadine Jurrmann, bioaccess® will support you with case number planning and analysis of your PMCF data, further emphasizing the collaborative effort needed in this process, particularly within the context of Latin America.
Insights from Industry Leaders: Best Practices and Lessons Learned
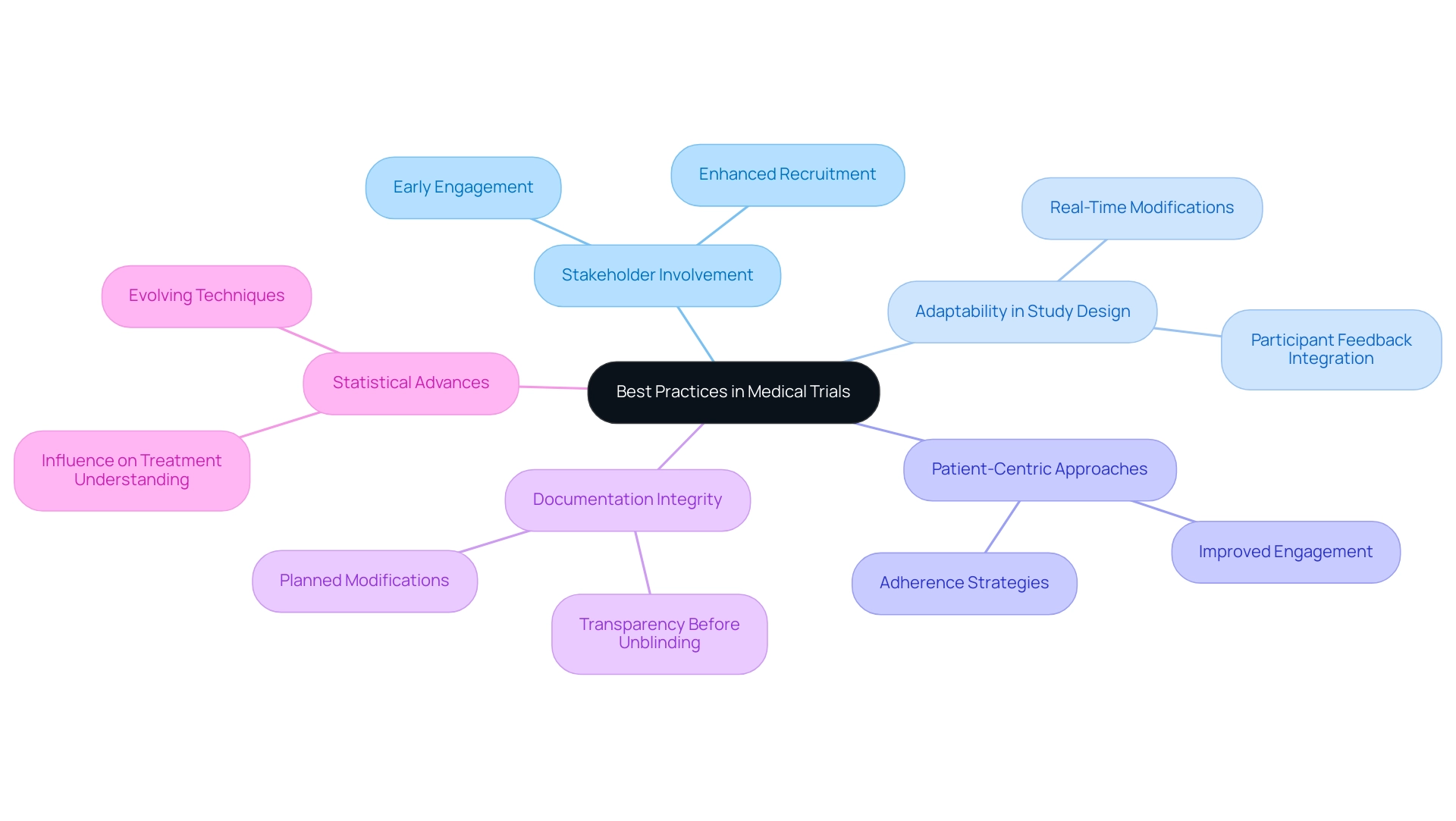
Insights from industry leaders underscore the critical role of early stakeholder involvement in conducting trials for breakthrough medical devices. Engaging stakeholders from the outset not only streamlines execution but also enhances recruitment efforts, ultimately leading to higher success rates. Furthermore, adaptability in study design is essential; it allows for real-time modifications based on information and participant feedback, significantly improving study outcomes.
It is imperative to document all planned modifications and analyses prior to data unblinding to uphold the integrity and transparency of the study.
A strong focus on patient-centric approaches is vital. Trials for breakthrough medical devices designed with the patient's experience at the forefront tend to yield improved engagement and adherence, which are crucial for achieving reliable results. By integrating these best practices, research directors can enhance the effectiveness and efficiency of their studies, facilitating quicker market access and better patient outcomes.
bioaccess® plays a pivotal role in connecting innovative Medtech companies with opportunities for conducting research studies in Latin America, providing a distinct value proposition that supports these best practices. Dushyanth Surakanti, Founder & CEO of Sparta Biomedical, shared his positive experience with bioaccess® during its first human study in Colombia, emphasizing the collaborative efforts that enhance execution. Moreover, the partnership between bioaccess™ and Caribbean Health Group aims to establish Barranquilla as a leading location for medical research in Latin America, with the backing of Colombia's Minister of Health, Juan Pablo Uribe.
This partnership, announced on March 29, 2019, is crucial for attracting more research projects to the region and has already shown promising results, including a significant reduction in recruitment time and high retention rates.
As Dr. Tao Chen, a senior lecturer in Biostatistics, notes, "Statistics, including its use in research design and analysis, is constantly advancing with ongoing technological progress." This evolution highlights the importance of research statistics as fundamental to medical studies, influencing treatment understanding and healthcare decisions.
As the landscape of medical research evolves, being attuned to these insights will enable organizations to navigate the complexities of study administration effectively. The historical context of ClinicalTrials.gov, established in 2000, further emphasizes the significance of clinical trials in the contemporary landscape, marking a pivotal advancement in the transparency and accessibility of clinical research.
Conclusion
Breakthrough medical devices are reshaping the healthcare landscape, offering innovative solutions that significantly enhance treatment outcomes for patients facing life-threatening conditions. The FDA's Breakthrough Devices Program plays a crucial role in fast-tracking these advancements, ensuring that patients have timely access to life-saving technologies. However, the journey from concept to market presents numerous challenges, particularly during the clinical trial phase, where regulatory compliance, patient recruitment, and effective collaboration are essential.
The article underscores the importance of strategic partnerships and innovative methodologies as vital components in overcoming obstacles encountered during clinical trials. Engaging diverse stakeholders—including healthcare providers, regulatory bodies, and patient advocacy groups—enriches the research process and fosters trust, ultimately leading to improved recruitment and retention rates. Furthermore, the implementation of adaptive trial designs and advanced data management techniques is critical for ensuring reliable outcomes and preserving the integrity of clinical studies.
In summary, the effective integration of breakthrough medical devices into clinical practice is essential for advancing healthcare and enhancing patient lives. By prioritizing collaboration, leveraging innovative strategies, and adhering to regulatory standards, the medical community can navigate the complexities of clinical trials more efficiently. As the demand for advanced medical technologies continues to rise, the commitment to fostering innovation and ensuring patient-centric approaches will be pivotal in transforming the future of healthcare.
Frequently Asked Questions
What are breakthrough medical instruments?
Breakthrough medical instruments are defined as those that provide more effective treatment or diagnosis for life-threatening or irreversibly debilitating diseases.
What is the purpose of the FDA's Breakthrough Devices Program?
The FDA's Breakthrough Devices Program is designed to expedite the development and review of innovative medical products, ensuring that patients have timely access to therapies that can significantly improve their quality of life.
How many Breakthrough Device designations were requested and granted in 2022?
In 2022, over 30 Step designations were requested, of which 14 were granted.
Why are breakthrough innovations significant in healthcare?
Breakthrough innovations symbolize major progress in medical technology, addressing unfulfilled healthcare requirements and improving patient outcomes.
What types of studies are important for breakthrough medical devices?
Clinical studies for breakthrough medical devices must be carefully crafted to accommodate their unique features, ensuring robust and pertinent information is gathered.
What services does bioaccess® provide for trial management?
Bioaccess® offers comprehensive trial management services, including Early-Feasibility Studies (EFS), First-In-Human (FIH) studies, Pilot Studies, Pivotal Studies, and Post-Market Follow-Up Studies (PMCF).
When should companies apply for Breakthrough Device Designation?
Companies should apply for Breakthrough Device Designation as soon as they can provide initial trial information demonstrating the feasibility of their device's performance in trials.
What recent regulatory changes have been noted regarding hearing aids?
The FDA is allowing some hearing aids intended for mild to moderate hearing loss to be sold over-the-counter (OTC) without the need for physician involvement.
How do groundbreaking medical instruments impact patient outcomes?
These tools enhance treatment efficacy, result in higher patient satisfaction, and improve quality of life.
What challenges exist in accessing breakthrough medical innovations?
Challenges include inconsistent coverage from private insurers and the lack of approved bills for immediate CMS coverage, which can hinder access to these vital innovations.
What is the importance of diversity in research trials according to recent FDA regulations?
The FDA mandates sponsors to submit Diversity Action Plans (DAPs) to enhance participant enrollment from historically underrepresented populations, improving the reliability of data and reflecting the demographics of the populations using the medical devices.
How can engaging regulatory consultants benefit research studies?
Engaging regulatory consultants early in the study design phase can ensure that all necessary documentation and compliance measures are meticulously addressed, paving the way for a smoother approval process.

