Overview
Leveraging technology for trial design significantly enhances clinical research by improving efficiency, patient engagement, and data integrity through tools such as electronic data capture, AI, and telemedicine. This article illustrates how these technologies streamline processes, reduce operational burdens, and facilitate participant involvement. Ultimately, these advancements lead to more successful and patient-focused outcomes in clinical trials. The integration of these technologies not only addresses existing challenges but also sets a new standard for future research methodologies.
Introduction
In the dynamic realm of clinical research, the integration of technology is revolutionizing trial design and execution. Organizations are increasingly focused on enhancing operational efficiency and improving patient engagement, making innovative tools like electronic data capture systems and mobile applications indispensable. These advancements streamline data collection while empowering researchers to prioritize participant experience in their trials.
With the emergence of artificial intelligence, wearable devices, and telemedicine, the future of clinical trials is on the brink of a significant transformation, promising more efficient and patient-centric methodologies. However, it remains crucial to navigate the ethical and regulatory challenges that accompany these technological innovations.
This article explores the pivotal role technology plays in clinical trial design, examines key innovations reshaping the landscape, and offers strategic insights for effectively leveraging these tools.
Understanding the Role of Technology in Clinical Trial Design
In the evolving landscape of medical research, leveraging technology for trial design is paramount for enhancing study design and implementation. Electronic data capture (EDC) systems streamline data collection processes, enabling real-time monitoring and analysis. This shift not only enhances operational efficiency but also significantly improves patient engagement.
By utilizing mobile applications, researchers can bolster participant recruitment and retention, providing timely updates and reminders that strengthen study compliance.
Researchers are harnessing technology for trial design through the incorporation of advanced analytics, which further enables them to create studies that are both efficient and patient-focused. Recent statistics reveal a surge in the implementation of innovations in study design, with numerous organizations reporting a marked increase in efficiency. For instance, the adoption of EDC systems has been shown to reduce the time spent on data entry and management, allowing clinical research associates (CRAs) to concentrate on critical tasks that enhance study integrity.
Moreover, ICH E6 R2 (and R3 revisions) mandates that sponsors manage risk in a manner that alleviates the burden on sites, underscoring the importance of innovation in refining study procedures.
Expert opinions underscore the significance of innovation in research design. A senior director in a global biopharma's research sciences group noted that eliminating a single 20-minute task per visit across 130,000 visits could save approximately 43,000 hours of effort, enabling CRAs to focus on what truly matters in the study process.
Real-world examples further illustrate the impact of innovation. The CureApp Smoking Cessation system, for instance, demonstrated improved long-term tobacco abstinence rates when combined with standard care, showcasing how innovation can enhance treatment outcomes. Furthermore, the COVID-19 pandemic has accelerated the adoption of digital tools in research studies, emphasizing their potential to uphold study integrity and participant safety through remote methodologies.
This transformation has highlighted the enduring significance of digital solutions in the research environment.
As we approach 2025, recent innovations are directed at leveraging technology for trial design to further revolutionize study design. The ongoing development of EDC systems and the integration of cloud-based tools will continue to enhance efficiency, ultimately bridging the gap between innovative Medtech companies and the vast potential for conducting research studies in Latin America. With bioaccess®'s 20+ years of experience in Medtech and expertise in managing Early-Feasibility, First-In-Human, Pilot, Pivotal, and Post-Market Follow-Up studies, the company stands poised to support this unique value proposition, driving global health improvement through international collaboration and innovation in Medtech.
Key Technologies Transforming Clinical Trials
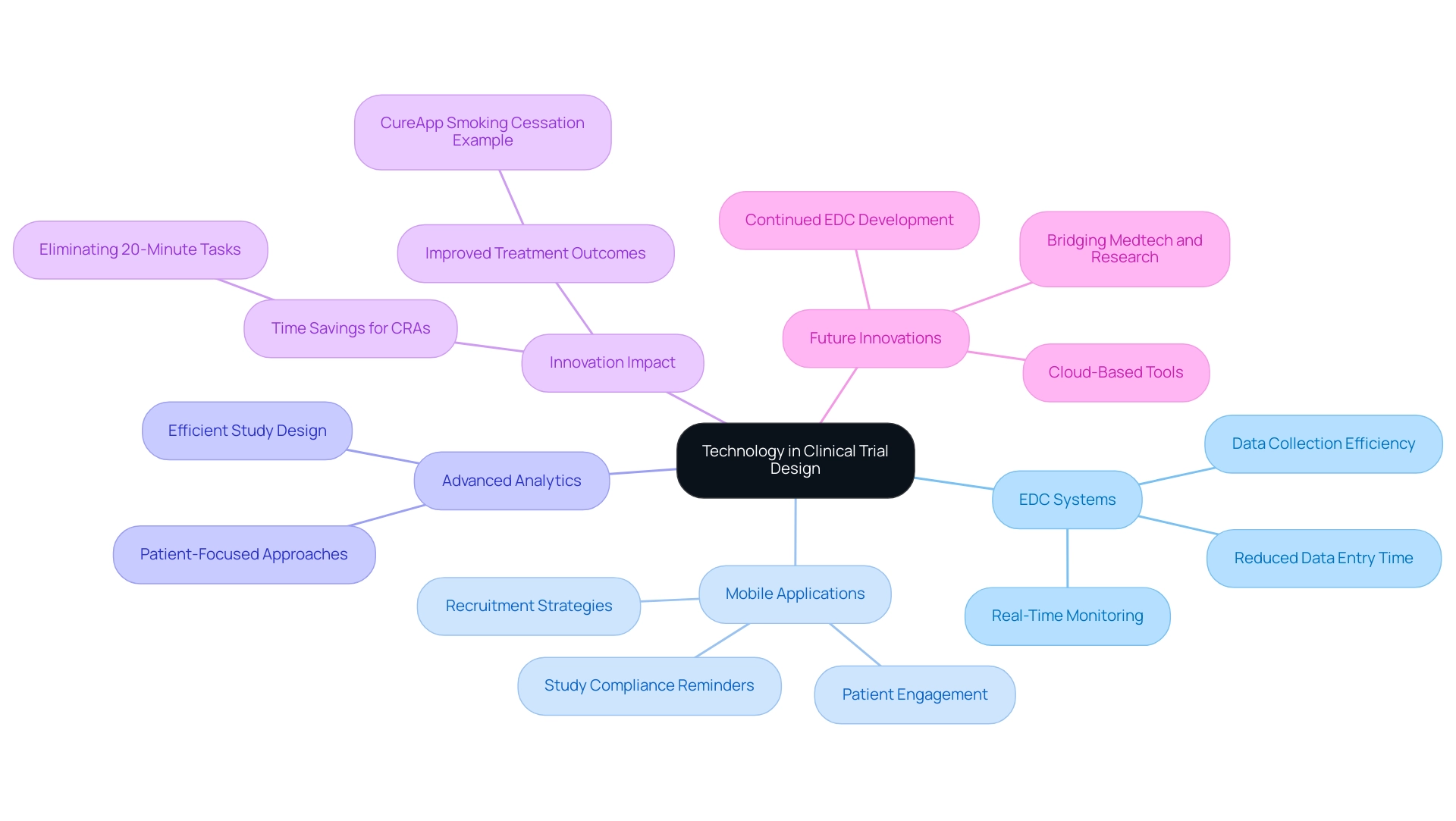
Leveraging technology for trial design is reshaping the landscape of clinical studies by enhancing efficiency and accuracy. Key advancements include:
- Artificial Intelligence (AI): AI's capability to analyze extensive datasets enables the identification of patterns and prediction of outcomes, which is crucial for optimizing patient selection and refining study design. Recent statistics indicate that while 51% of U.S. adults are optimistic about AI's potential to drive healthcare advancements, there remains a significant trust gap, with 75% of patients expressing skepticism about AI's role in healthcare settings. Addressing these ethical concerns, particularly regarding information privacy and informed consent, is essential for broader acceptance. A significant instance is the collaboration between IBM Watson Health and Bristol Myers Squibb, which seeks to incorporate artificial intelligence into research processes to expedite patient recruitment and enhance information analysis.
- Wearable Devices: The incorporation of wearable devices enables ongoing observation of patient health metrics, producing immediate insights that greatly improve research precision. Current trends show an increasing adoption of these devices, which not only enhance information collection but also empower patients to take an active role in their health management during trials.
- Telemedicine: The rise of telemedicine has revolutionized patient engagement by providing virtual consultations that enhance accessibility and convenience. This change enables participants to stay linked to the process without the obstacles of travel, thus enhancing enrollment and retention rates.
- Blockchain: This innovation plays a crucial role in ensuring information integrity and security, which are essential for upholding trust in medical research. By offering a clear and unchangeable record of transactions, blockchain can assist in addressing worries about privacy and informed consent, which are crucial ethical factors in medical studies. Moreover, the FDA's requirement for the approval of new digital biomarkers prior to their application in machine learning processing of device information highlights the regulatory factors that influence the use of AI in research studies.
Leveraging technology for trial design simplifies study workflows and promotes a more patient-focused approach, ultimately resulting in more successful outcomes in research. At bioaccess®, we leverage our 20+ years of expertise in managing clinical studies, including Early-Feasibility Studies (EFS), First-In-Human Studies (FIH), Pilot Studies, Pivotal Studies, and Post-Market Follow-Up Studies (PMCF), to ensure that our clients navigate the complexities of study design and execution with confidence. Additionally, our commitment to data protection and transparent grievance procedures ensures that client concerns are addressed promptly and in compliance with applicable laws.
Integrating Digital Solutions into Trial Operations
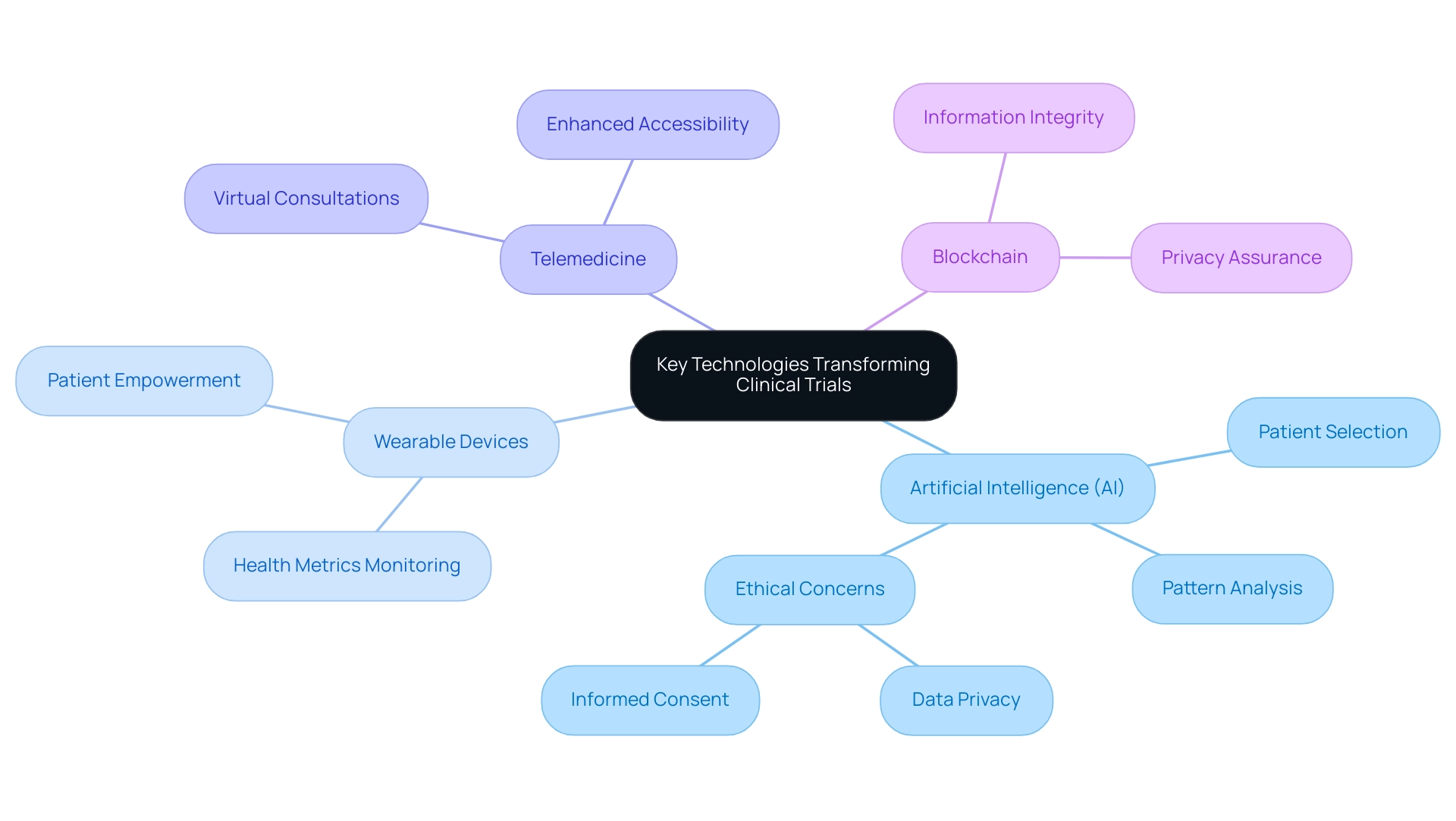
Leveraging technology for trial design in testing operations necessitates a methodical approach to ensure both efficiency and effectiveness, particularly within the Latin American Medtech landscape. Begin by thoroughly evaluating existing workflows to pinpoint areas where technology can significantly enhance operational efficiency. This evaluation should focus on recognizing bottlenecks and opportunities for enhancement, especially by utilizing technology for trial design in clinical studies across Latin America.
Select digital solutions that align well with the specific objectives of your experiment. For instance, implementing Electronic Data Capture (EDC) systems streamlines data collection, while patient engagement platforms enhance participant interaction and retention. bioaccess® provides customized solutions that facilitate these processes, ensuring evaluations are conducted smoothly and efficiently.
Comprehensive training for all team members on the new technologies is crucial. This preparation ensures that everyone can effectively utilize the tools, maximizing their potential to improve outcomes. bioaccess® emphasizes the importance of training in their research management services, guaranteeing that teams are well-prepared to harness advanced technologies.
Continuously monitor the integration process to identify any challenges that may arise. Regular evaluations allow for prompt modifications, ensuring that the tools are being utilized to their fullest extent. The expertise of bioaccess® in managing health studies, including Early-Feasibility and First-In-Human research, supports effective monitoring and adaptation of study operations.
The efficacy of these digital solutions is underscored by recent statistics, which reveal that 95% of participants expressed satisfaction with interventions focused on leveraging technology for trial design. Moreover, historical trends indicate a significant shift in the research environment; for example, the pandemic accelerated the adoption of electronic Investigator Site Files (exISts), with 89% of sites anticipating their use by early 2022, up from 61% just two years earlier. This rapid adoption of advancements, including eConsent and remote monitoring, highlights the necessity for research organizations to adapt and innovate by leveraging technology for trial design.
As bioaccess®, a leading contract research organization in Latin America, points out, their expertise and tailored approach aim to expedite medical devices, providing valuable solutions for the Medtech sector. Furthermore, the U.S. FDA has issued guidance for sponsors, researchers, and IRBs regarding the use of electronic informed consent, emphasizing the importance of regulatory adherence in the integration of digital solutions.
By adhering to these strategic measures, researchers can establish efficient and impactful study operations, ultimately leading to enhanced outcomes and a competitive advantage in the evolving research landscape.
Navigating Ethical and Regulatory Challenges
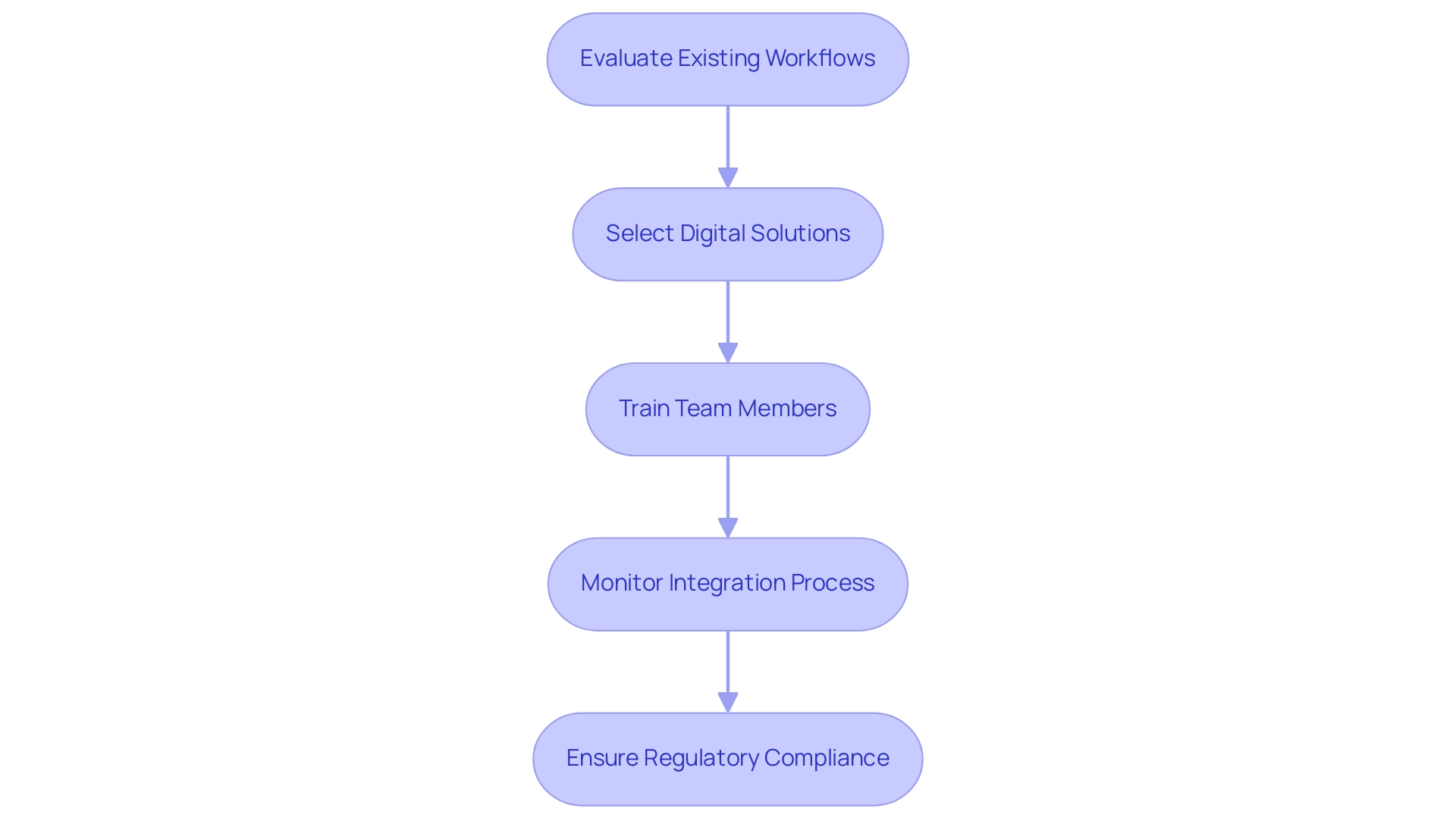
Incorporating innovation into clinical studies presents researchers with a variety of ethical and regulatory hurdles that must be approached cautiously. Informed Consent is paramount; participants must have a clear understanding of how their information will be utilized and the implications of the study's methods. A recent study indicated that the use of telemedicine for electronic informed consent (e-IC) was deemed acceptable by legally authorized representatives of stroke patients, signaling a shift towards more flexible consent processes in technology-driven research. This acceptance underscores the growing integration of digital health innovations, evidenced by a PubMed search revealing 5,287 randomized controlled trials related to health and digital health.
Information Privacy is another critical area, where robust protection measures are essential to safeguard participant details. Compliance with regulations such as GDPR and HIPAA is non-negotiable. As digital health innovations proliferate, concerns regarding information privacy have intensified, necessitating stringent protocols to protect sensitive details. For instance, a systematic review of methodologies for evaluating e-IC highlighted the importance of comprehensive data privacy measures to enhance participant trust and engagement. This aligns with bioaccess's commitment to accelerating the development of medical devices through its expertise in extensive research management services, including compliance assessments, project oversight, feasibility evaluations, site selection, and setup. Researchers must ensure that all technological tools employed in experiments meet the necessary standards. As we look toward 2025, the moral dilemmas related to innovations in medical studies continue to evolve, with specialists emphasizing the necessity for clear protocols to manage these complexities effectively. Katherine Ruiz, a specialist in regulatory matters for medical devices and in vitro diagnostics in Colombia, underscores the significance of adhering to these guidelines, as they are essential for preserving the integrity of research.
By actively addressing these issues, researchers can cultivate trust among participants and ensure the ethical management of their studies, ultimately promoting the advancement of medical devices and enhancing patient outcomes.
Evaluating the Benefits and Limitations of Technology in Trials
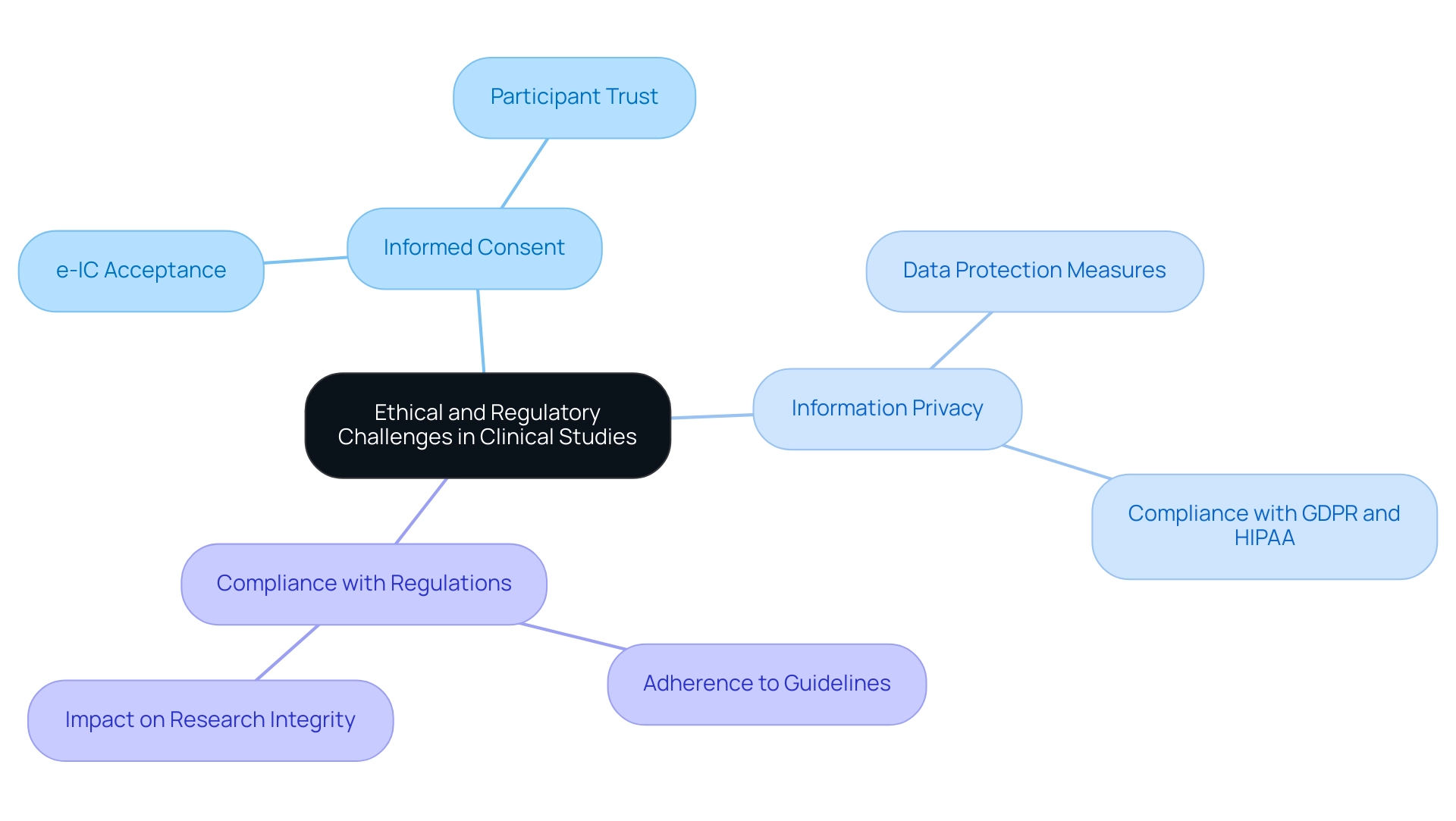
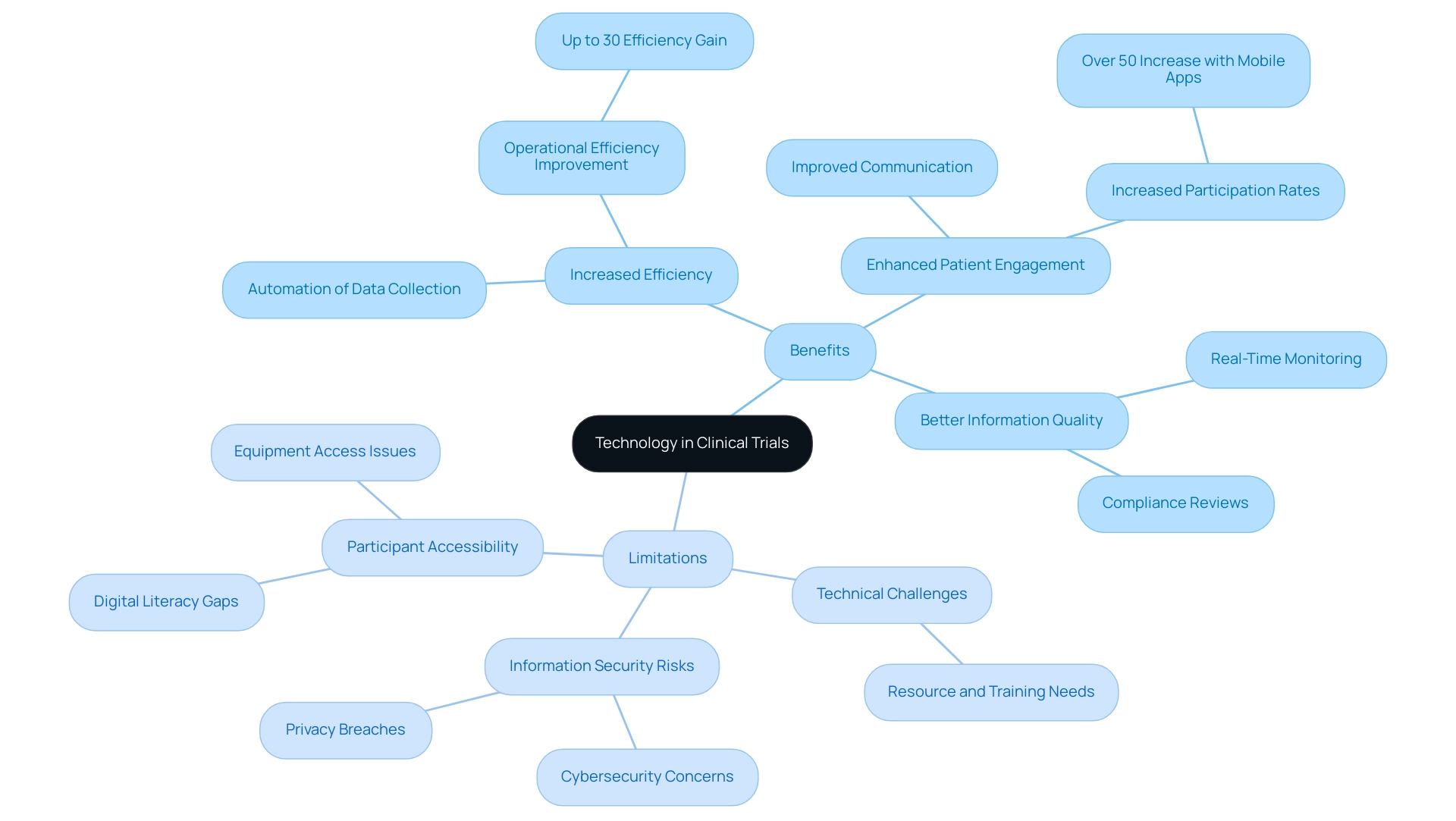
The integration of technology in clinical trial design brings a wealth of advantages, yet it is essential to recognize the accompanying limitations:
Benefits:
- Increased Efficiency: Automation of data collection and analysis can significantly shorten trial timelines, with studies indicating that technology can enhance operational efficiency by up to 30% in clinical trials. The healthcare companies segment dominated the market with the largest revenue share of 43.75% in 2024, underscoring the growing importance of technology in this field. bioaccess® provides extensive clinical study management services, including feasibility studies, site selection, setup, import permits, and reporting on adverse events, which further streamline these processes.
- Enhanced Patient Engagement: Digital tools foster improved communication and participation rates among patients, with recent findings showing that patient engagement rates can increase by over 50% when utilizing mobile health applications. Wilhelm and colleagues describe ways to use the Internet, phones, and apps to provide cognitive-behavioral therapy to those with mental health disorders, illustrating the potential of digital tools in enhancing patient involvement.
- Better Information Quality: Real-time monitoring and information collection contribute to more accurate and reliable results, ensuring that integrity is maintained throughout the trial process. bioaccess® emphasizes compliance reviews and project management to uphold these standards.
Limitations:
- Technical Challenges: The implementation of new technologies often necessitates substantial resources and training, which can pose hurdles for clinical research teams, particularly in smaller organizations.
- Information Security Risks: As dependence on digital tools increases, so do concerns regarding breaches and privacy. Ensuring robust cybersecurity measures is critical to protect sensitive patient information. bioaccess® is dedicated to information protection, addressing client concerns through established grievance procedures and providing contact details for the Grievance/Information Protection Officer to ensure compliance and transparency.
- Participant Accessibility: Not all patients may have access to the required equipment, which can limit involvement and distort study demographics. This is particularly relevant in regions where digital literacy and access to devices are unevenly distributed.
Furthermore, the ethical factors and information standards essential for carrying out medical studies that employ digital methods are vital. A recent case study titled "Ethical Considerations in Digital Clinical Trials" emphasizes the importance of establishing clear ethical guidelines and data standards to ensure participant safety and data integrity. Moreover, there is clearer direction from ethics and regulatory organizations on integrating digital tools in medical studies, which is essential for navigating the changing environment.
By thoughtfully assessing these advantages and drawbacks, medical researchers can make knowledgeable choices regarding leveraging technology for trial design, ultimately enhancing the implementation of studies. Present uses of AI in healthcare, such as experiments for antibiotic dosing and intraoperative hypotension management, further demonstrate the practical role of innovation in advancing medical research.
Step-by-Step Strategies for Leveraging Technology
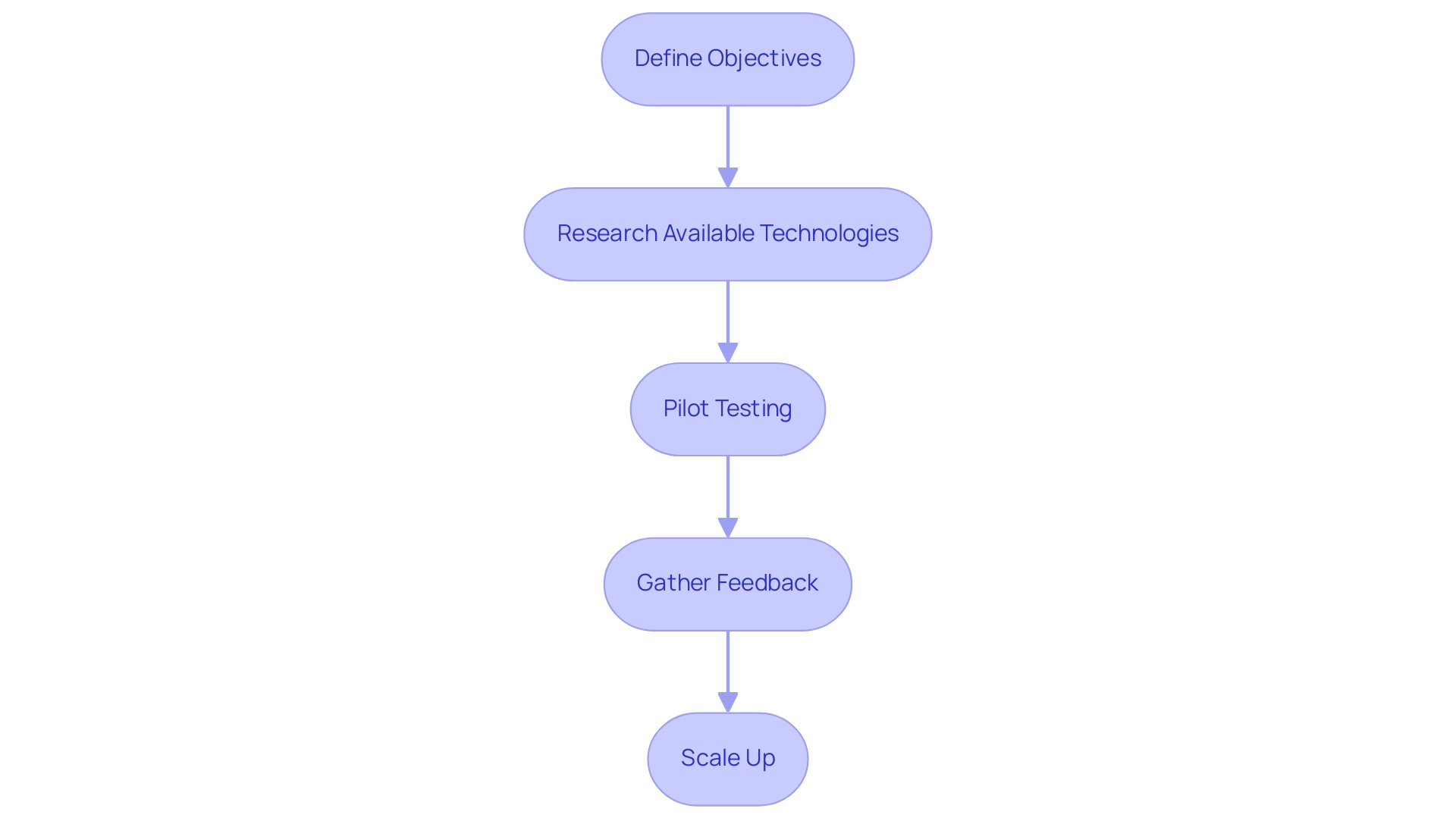
To effectively leverage technology in clinical trial design, it is essential to consider comprehensive strategies that ensure success:
- Define Objectives: Clearly outline the specific goals of the experiment. Understanding how innovation can enhance these objectives is crucial for successful integration.
- Research Available Technologies: Explore a range of tools and platforms that align with your study's requirements. This includes investigating advancements such as wearable devices, which have been effectively utilized by companies like ObvioHealth to collect real-time health information and track vital signs. This facilitates faster identification of safety signals associated with treatments. Additionally, contemplate the potential of blockchain systems to enhance data integrity and safety in medical studies.
- Pilot Testing: Conduct pilot tests of selected methods to evaluate their effectiveness. This step is vital for identifying potential issues before full-scale implementation. Data from pilot testing results can provide insights into the success rates of system integration in clinical studies, assisting in refining your approach.
- Gather Feedback: Collect input from test participants and staff regarding their experiences with the device. This feedback is invaluable for refining the use of tools and ensuring they meet the needs of all stakeholders involved.
- Scale Up: After validating the system through pilot testing and feedback, implement it across the experiment. Ensure that all team members receive adequate training and support to maximize the advantages.
By leveraging technology for trial design, researchers in the medical field can fully utilize the capabilities of innovation in their study designs, ultimately resulting in more effective workflows and enhanced outcomes. As bioaccess® emphasizes, their expertise in managing trials—including Early-Feasibility, First-In-Human, Pilot, Pivotal, and Post-Market Follow-Up Studies—is backed by over 20 years of experience in Medtech, positioning them as a valuable partner in navigating the complexities of research in Latin America. As Carmen Rosa from the National Institutes of Health remarked, "This public health crisis has further emphasized the opportunities for utilizing digital tools in medical research and practice."
As the landscape of medical investigation evolves, incorporating sophisticated tools will be essential to remaining at the forefront of the field. Moreover, with IDC forecasting that under 5% of all data created electronically will be assessable by 2025, the significance of utilizing advancements effectively in medical studies cannot be overstated. By embracing these advanced innovations, researchers can ensure they are prepared for the challenges ahead.
Future Trends in Technology-Driven Clinical Trials
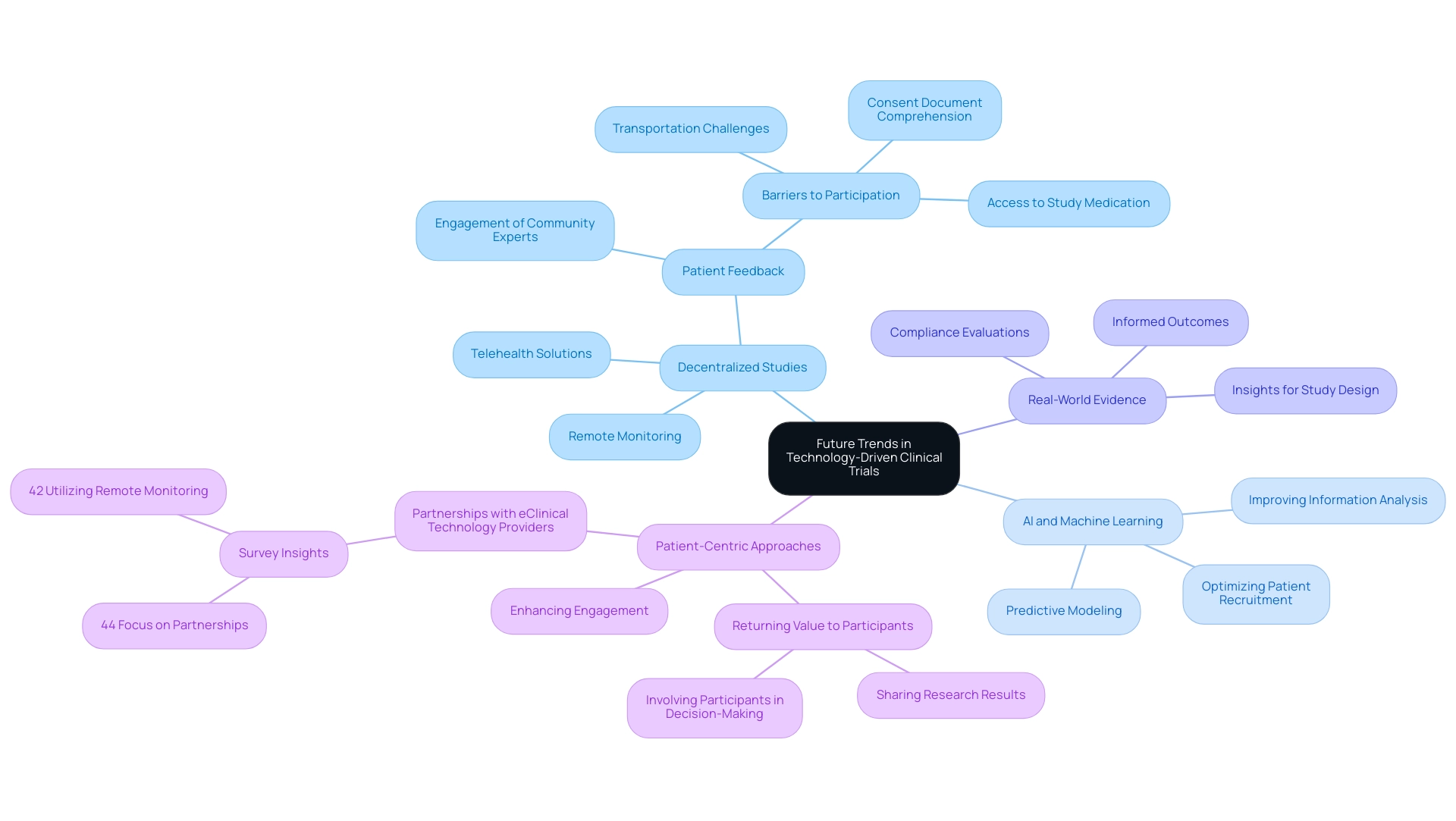
As technology continues to evolve, several key trends are poised to shape the future of clinical studies, particularly through the comprehensive services offered by Bioaccess.
Decentralized Studies: The increasing adoption of remote monitoring and telehealth solutions is revolutionizing participation. This shift not only enhances accessibility for patients but also addresses common barriers to participation, such as transportation challenges and the complexities of consent processes. Bioaccess supports this transition by providing feasibility studies and site selection, ensuring that studies are designed with patient accessibility in mind. A notable example is the PREVENTABLE study, which engaged eight community experts aged 75+ years to review the protocol, highlighting the importance of participant feedback in study design. Key obstacles to possible study involvement included transportation to research visits, difficulty comprehending the consent document, and access to study medication.
AI and Machine Learning: These advanced technologies are set to play a crucial role in optimizing research studies. From optimizing patient recruitment to improving information analysis and predictive modeling, AI and machine learning are anticipated to greatly enhance efficiency in studies. Bioaccess utilizes these tools to improve project management and reporting, enabling more accurate targeting of patient populations and better resource distribution throughout the study process.
Real-World Evidence: The inclusion of real-world data is becoming increasingly essential in medical research. This trend enables researchers to gain insights that can inform study design and outcomes, ultimately leading to more relevant and impactful results. As biopharmaceutical sponsors invest in decentralized studies, the use of real-world evidence will likely grow, offering a richer context for understanding patient experiences and treatment effects. Bioaccess's expertise in compliance evaluations, study setup, and reporting on serious and non-serious adverse events ensures that research is aligned with these evolving standards.
Patient-Centric Approaches: Future studies will prioritize patient experience, utilizing advancements to enhance engagement and satisfaction. This shift towards a more patient-centric model is reflected in the growing emphasis on returning value to participants, such as sharing research results and involving them in the decision-making process. According to ISR's 2022 survey, 44% of respondents indicated a focus on establishing partnerships with eClinical technology providers, demonstrating a strong commitment to decentralization. Bioaccess's comprehensive project management services facilitate this engagement, ensuring that patient needs are at the forefront of trial design, especially by leveraging technology for trial design. By staying informed about these trends and leveraging technology for trial design through the comprehensive clinical trial management services offered by Bioaccess, clinical researchers can strategically prepare for the evolving landscape of clinical trials. This approach not only improves outcomes and patient experiences but also contributes to local economies through job creation and healthcare improvement, fostering international collaboration in the field.
Conclusion
The integration of technology in clinical trial design signifies a transformative shift towards more efficient and patient-centric methodologies. As explored throughout this article, tools such as:
- electronic data capture systems
- artificial intelligence
- wearable devices
- telemedicine
are enhancing operational efficiency and fundamentally reshaping patient engagement. The capacity to collect real-time data and maintain participant connectivity has proven invaluable, particularly in light of the challenges posed by the COVID-19 pandemic.
However, these advancements also introduce ethical and regulatory challenges. Ensuring informed consent, safeguarding data privacy, and adhering to evolving regulations are critical for maintaining trust and integrity in clinical research. Proactively addressing these issues is essential for fostering participant confidence and advancing medical innovations.
As the landscape continues to evolve, embracing future trends such as:
- decentralized trials
- real-world evidence
- a focus on patient-centric approaches
will be crucial. By leveraging these technologies and strategies, researchers can enhance the design and execution of clinical trials, contributing to better health outcomes and improved patient experiences.
Ultimately, the commitment to integrating advanced technologies within clinical trials heralds a new era in healthcare research. By staying attuned to these developments, clinical researchers can navigate the complexities of trial design with confidence, ensuring they remain at the forefront of innovation in the Medtech sector.
Frequently Asked Questions
How is technology being leveraged for trial design in medical research?
Technology is enhancing trial design by streamlining data collection through Electronic Data Capture (EDC) systems, improving operational efficiency, and boosting patient engagement.
What role do mobile applications play in clinical trials?
Mobile applications aid in participant recruitment and retention by providing timely updates and reminders, which strengthen study compliance.
What impact do advanced analytics have on study design?
Advanced analytics enable researchers to create efficient and patient-focused studies, leading to increased efficiency in clinical trials.
How do EDC systems improve the data management process?
EDC systems reduce the time spent on data entry and management, allowing Clinical Research Associates (CRAs) to focus on critical tasks that enhance study integrity.
What are the implications of ICH E6 R2 (and R3 revisions) for clinical trials?
These revisions mandate that sponsors manage risk in a way that alleviates the burden on sites, emphasizing the importance of innovation in refining study procedures.
Can you provide an example of how innovation has positively impacted clinical research?
The CureApp Smoking Cessation system demonstrated improved long-term tobacco abstinence rates when combined with standard care, illustrating how innovation can enhance treatment outcomes.
How did the COVID-19 pandemic influence the adoption of digital tools in research?
The pandemic accelerated the use of digital tools in research studies, emphasizing their potential to maintain study integrity and ensure participant safety through remote methodologies.
What advancements in technology are expected to shape trial design by 2025?
Innovations such as the ongoing development of EDC systems and the integration of cloud-based tools are expected to enhance efficiency and bridge gaps in research studies.
What technologies are highlighted as key advancements in clinical trials?
Key advancements include Artificial Intelligence (AI), wearable devices, telemedicine, and blockchain, each contributing to improved patient engagement and data integrity.
How does AI contribute to optimizing clinical trials?
AI analyzes extensive datasets to identify patterns and predict outcomes, which is crucial for optimizing patient selection and refining study design.
What benefits do wearable devices offer in research studies?
Wearable devices allow for ongoing observation of patient health metrics, providing immediate insights that enhance research precision.
How has telemedicine changed patient engagement in clinical trials?
Telemedicine provides virtual consultations that enhance accessibility and convenience, allowing participants to remain engaged without the need for travel.
What is the role of blockchain in medical research?
Blockchain ensures information integrity and security by offering a clear and unchangeable record of transactions, addressing privacy and informed consent concerns.
How does bioaccess® leverage its expertise in managing clinical studies?
Bioaccess® utilizes over 20 years of experience to navigate the complexities of study design and execution, ensuring compliance with data protection and grievance procedures.

